Left Ventricle Assist Device, THE LVAD. This device would change our lives forever. We had never even heard of it before. It was now in my husband and it would be our new normal way of living. When I say ours, it may be in Joe but it takes the two of us for him to survive.
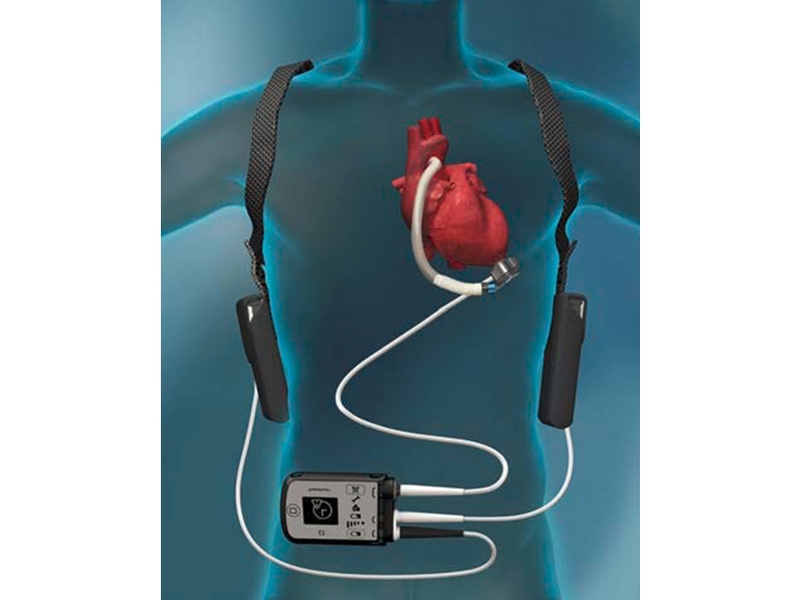
This device is a mechanical pump that is attached to the left side of Joe’s heart. It’s purpose is to pump the blood from the lower left chamber of his heart to the rest of his body. The pump has a driveline that comes out of an open wound in Joe’s stomach. The driveline is attached to a controller. The controller also has two cords that are connected to batteries during the day and then connected to a power source unit at night or when he is sleeping. This LVAD will stay connected to Joe until he can get a heart transplant. They call it a Bridge to Transplant.
The batteries running the LVAD will last approximately 14 hours depending on Joe’s activity. The more you’re active the sooner the batteries will wear down. There is a button on the batteries that you can push to see how much battery life is remaining. If the batteries get low on life an alarm will sound to let you know. When this happens you have to switch to fully charged batteries or switch to the power source. There is also a charging station to keep all batteries at 100% charged.
We have a bag with four extra batteries and a spare controller. We must take this bag with us wherever we go. We can’t leave it in the car, it must be with us at all times. It is like a life line for Joe. If the batteries were to die or the controller was to go bad, we have that bag with all the spare items we need. Its not to be taken lightly, if you forget the bag a home you should go get it before doing anything. We left it once and vowed never to forget it again.
We have developed a routine, even before we left the hospital we had a plan in place. We have four sets of batteries that we rotate each day according to their number. So we always have three sets fully charged. Joe wears the batteries in a harness with one on each of his sides. The controller fits in a case that is attached to a belt.
On the controller is a digital screen which has the 4 P’s of the LVAD. 1. Pump Flow is an estimate of cardiac output based on pump speed and power. It typically ranges from 4 to 6 L/minute. Pump flow is influenced by mean arterial pressure (MAP); a higher MAP increases pump flow, and a lower MAP decreases it. Joe’s pump flow is usually 3.5. 2. Pump Speed indicates the speed at which the LVAD rotors are spinning. The usual range is 8,600 to 9,800 rpm. The doctors set Joe’s speed at 5200 because that number worked best with his heart. 3. Pulse Index (PI) is a measurement of flow through the pump and is determined by pump speed and the patient’s native heart function. PI typically ranges from 3 to 7. Lower values reflect less native heart function and greater reliance on the pump, while higher values reflect more native heart function and less support by the pump. Joe’s PI is usually 4.0 to 5.6 4. Power is the amount of wattage the device needs to maintain speed and flow. The normal range is 4 to 7 W. Joe’s power usually reads 3.9 to 4.0. Everyday morning I record all of his numbers (as we call them) just to keep track for myself. It helps ease my mind know what they were from day to day. I usually check them periodically during the day and before we go to bed.
The controller also has a lot of alarm codes we have to watch out for, if an alarm goes off we have to first check the controller and then call our LVAD team right away to let them know. We have only had two alarms since implant on 9-26-19, one was when Joe was connected to power and there was a power outage on our block. We just switch to batteries quickly until the power was restored. The other was a low flow alarm. This alarm can go off for many reasons. The team felt that he may of been a little dehydrated (dry). We just had Joe drink more water that day and he was fine. All alarms will display on the controller. In the manual is a list of what they mean and how to address them. Scary as it may seem, it’s now just something we have learned to accept. Just like changing oil or getting gas in your car. You just do it.
The Driveline that comes out of Joe’s stomach is considered an open wound and has to be cared for. While we were in the hospital and when we first came home the dressing on the driveline had to be changed every three days. Now that it is healed, we only have to change it every seven days. I check the site every night to make sure it looks good and there is no infection or redness. If this site becomes infected, the infection could do straight up the line into his heart. If this were to happen it would involved having the pump replaced with a new one. Another open heart surgery. So I stay on top of this because I do not want that to ever happen. This to me is the most important job I have as Joe’s caregiver.
There is a lot to learn about this LVAD. I have read the manual and have been instructed by the LVAD team. There is so much more to learn and I make it a point to read on it and research things so I am fully aware of all the information out there. My husband will always have a good support system with me on board because Knowledge is Power. I will always keep learning no matter what. LVAD STRONG!
Leave a comment